'A scary journey': Woman unknowingly suffers stroke while pregnant with twins
Anna De Souza, an American broadcast journalist, shared her personal story in honour of National Stroke Awareness Month in the US.

“You’re not imagining things, there’s definitely something going on there,” the resident at Wills Eye Center, one of the top eye hospitals in the country, told me during my second emergency room visit in 24 hours. I was pregnant with twins, experiencing neurological symptoms, and just 36 years old — and only at the very beginning of a scary journey, as it would take three months and several weekly doctor’s appointments to determine that I’d had a stroke.
But first, let’s rewind.
Pregnancy, then a death
After two rounds of back-to-back IVF cycles, we transferred one normal, high-grade, five-day embryo, which split into two. I was expecting identical twins! Even after the initial panic of a higher-risk pregnancy settled in, my excitement was tempered, since I had previously suffered two miscarriages.
Still, I felt lucky to have been able to share that first ultrasound photo of the two teensy circles that would eventually become my daughters with my mum, who passed away just three days later. She had been in and out of the hospital for three months, having suffered three strokes, the last of which painfully robbed her of speech.
That final month with her, during which I slept on a hospital recliner, I’d make my way to the communal restroom at 7 am to administer shots of progesterone in oil to my own buttocks. The oil was peanut buttery thick and my husband and I would warm it in our hands to help it move out of the syringe a bit easier. The meds would continue until I hit a few pregnancy benchmarks.
Then, in the midst of that, was my mother’s death, which shattered me. I was inconsolable, and, in many ways, I still am. Two weeks after her passing I was back home in Philadelphia for the first time in months, nearly 10 weeks pregnant. I took a deep breath and settled in.

Symptoms
The next morning at 5:30, my husband turned the closet light on. “Wow, I think I’m having a migraine,” I moaned. The centre of my right eye had a strange, glittering, grey gap in the shape of a vase, taking up about 25 per cent of my frontal vision. I couldn’t see anything through it, and it was as if that area was greyed out.
I have a history of migraine with aura — when a visual disturbance flickers around your central vision for about 20 minutes before a painful headache is triggered. The scariest part for me is feeling like it might never go away, and I’d always call my mum for comfort, no matter where I was. This time I couldn’t.
I can typically feel a migraine on the horizon two to three days before the onset of the aura. There are neurological symptoms. I’ll oftentimes have a hard time stringing words together, and it feels as if my neural functioning has slowed and I’ll find myself struggling to finish a thought. It’s often imperceptible to others, but my brain feels slower and I feel as if I’m stuttering. During the aura phase, I also feel like I can’t make sense of words around me. (Imagine looking at a stop sign knowing it says “stop," but just being able to perceive the “ST,” for instance.) Migraines also mess with my other senses, too, making everything smell pungent and bitter for days prior to a big episode. Post migraine I’ll have what I call the “migraine hangover,” where, for two days, my brain still feels achy and my senses finally begin to slowly reload.
That morning I sat in bed, then eventually ate breakfast, reasoning that maybe my sugar was low. Three hours passed, though, and the grey shape still blocked my vision. It threw off my depth perception. Finally, I called my husband and headed to the ER.
The investigation
Want to set off a circus? Head to the ER with neurological symptoms, pregnant with twins. For hours, my room became a rotating door of specialists. Initially, there was chatter about multiple sclerosis and optic neuritis. But then doctors were stumped, and at the end of a very long day, sent me home with steroids, no answers, and stubborn partial blindness in my right eye.
I called my neurologist the following morning, and he urged a visit to Wills Eye Hospital. That emergency department was packed and we were finally seen at 3 am. That’s when the resident told me, “You’re not imagining things, there’s definitely something going on there,” explained the resident, referring me to a neuro-ophthalmologist.
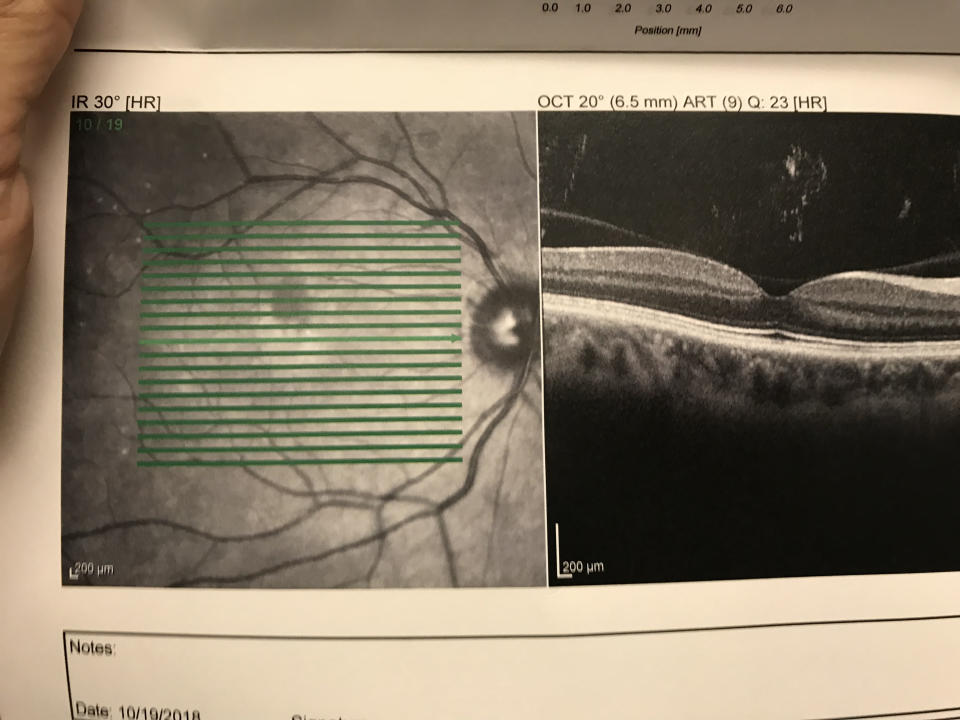
It wasn’t until three months later when the story finally came together. By that point I joked that I was seeing every “ologist” at Jefferson Health and Wills Eye Hospital. I was averaging three appointments weekly, coupled with obstetrics ultrasounds, as my pregnancy had become even higher risk with a slew of other complications.
I was referred to hematology, and my workup revealed higher than my normal cholesterol levels. Alarmed, my doctor immediately called to make a cardiology appointment for me. Good thing, because while it’s normal for cholesterol levels to rise during pregnancy, this serendipitous move was what ultimately puzzle-pieced together this mystery once and for all.
The perfect storm
My ultrasound revealed a PFO, short for “patent foramen ovale,” or a hole in the heart, something that more than a quarter of the population has. As a fetus, this hole allows blood to bypass the lungs which don’t work until they are exposed to air. For the majority of those with a PFO, blood leaks from the right to the left atrium without a problem — that is, until a blood clot comes into play.
"When you have a small communication between the two chambers of the heart where a small blood clot can get from the right side to the left side, that's when it can account for a stroke or an embolus to a part of the body, like a kidney or a finger, or even something like in your state where it went to one of the retinal arteries,” explains Dr Nicholas Ruggiero, cardiologist at Jefferson Health.
IVF medications, coupled with twin pregnancy, had created a perfect storm. A small clot that may have formed in my arms or legs and ordinarily would have been filtered by my lungs, undetected, instead crossed over in the PFO and travelled to my retina, which is technically part of your brain. This retinal occlusion happened painlessly, overnight, and cut off circulation to that area of my eye permanently.
The verdict? I had suffered a retinal stroke.
Still, such an embolic event affecting vision wasn’t always treated as a stroke. “Many times before people were just told it's a retinal artery occlusion, go home, maybe take aspirin, but now we treat them much more aggressively,” Ruggiero adds.
I couldn’t believe it. My mother’s three strokes were in part due to her own PFO, so I was already familiar with the etiology of this. I just couldn’t believe in many ways that we shared the same fate, though in different ways.

The here and now
I’m now treated with aspirin therapy, and when the pandemic restrictions lift, my PFO will be closed. I am worried. The risk is very small, but surgery could potentially trigger atrial fibrillation or even another stroke. While the fear to tackle this now is paralyzing, I know that the older I get, the more likely I am to develop another blood clot. Closing it now while I’m young and healthy is my best bet for avoiding bigger complications down the line.
The occlusion’s border is fuzzier now but still lies nearly dead centre in my field of vision, making it a daily nuisance. Looking at geometric shapes is a head trip. Window blinds and pedestrian crosswalk lines are the worst. Imagine seeing a straight line, then a gap, then the remainder of the line.
My brain has gotten better at putting together more organic shapes, like faces, for instance. Both eyes open fills in the gap, but if I look into a mirror with my left eye closed, nearly 20 per cent of my face is greyed out. I remember once joking about the challenges of applying eyeshadow to my left eye — silly but true.
I am grateful that with some adjustments I’ve been able to go on with my regularly scheduled life. I move my phone around a bit more to read emails, I lift the blinds in the living room every morning. It feels eerily ironic to me, though, that the one thing I always feared, an aura that just won’t go away is the reality I’m living with every time I blink my eyes. Interestingly enough, I’ve never cried over this, even in the height of uncertainty. I credit that to my mum, who, in the face of fear, put her game face on, too.

I truly never considered this would happen to me at such a young, but it’s happening to younger and younger people.
“Specifically in young, healthy people who have sudden blindness or difficulty with vision in an eye, a stroke should be a diagnosis that is entertained,” explains Ruggeiro.
“Most of the time when we talk about strokes, we're thinking about an older population and we're thinking about people with high blood pressure or diabetes or heart disease or other conditions,” adds Dr Jason Baxter, Maternal Fetal Medicine Specialist at Jefferson Health.
"I have multiple stories identical to this about young, healthy people who've had strokes,” Ruggerio continues. A lot of times, the inciting event is extraneous estrogen, either from an oral contraceptive pill, especially for smokers, or women who have had IVF, he explains, which comes with a thrombotic risk.
“Twin pregnancies increase that risk, but the real-time of risk for blood clots is in the postpartum period and the weeks after delivery,” warns Baxter. Women normally clot more post-birth to prevent excessive bleeding during and after delivery.

Baxter adds that my symptoms didn’t line up with F.A.S.T., the acronym used as a mnemonic to help detect strokes, standing for: facial drooping, arm weakness, speech difficulties and time to call emergency services. Despite this unusual presentation, I was lucky enough to get help and get placed on a preventative aspirin treatment. Once the diagnosis was made, my postpartum care included six weeks of Lovenox shots to prevent blood clots.
It’s critical that even during a pandemic, where fear of contracting COVID-19 is acute, that if you’re presenting with any facial drooping or other telltale signs of stroke that you head to the ER immediately. Any sudden changes in vision should also be investigated and diagnosed, therapies are available to mitigate any further episodes that could be even more catastrophic.
In the end, my high-risk pregnancy posed ups and downs right up until the birth — including a leg swelling right before delivery that prompted a stressful, pre-C-section ultrasound to confirm a blood clot wasn’t to blame (it wasn’t, thankfully).
But then, on the morning of April 4th, 2019, two healthy identical twin girls “sang” loudly upon entry into the world, reassuring me everything was going to be okay. They are well, meeting all of their milestones, and have wickedly silly giggles and endearing “twin talk” that echoes happily throughout the house. Life is really nice and I’m grateful that medical crises have been replaced with sloppy baby kisses and mundane chores like moving the couch to find missing wooden puzzle pieces.
I’ve certainly learned a lot from this experience. I’ve learned to advocate for myself as a patient, and that working in partnership with your care providers is crucial. I’m grateful to have been cared for so lovingly by so many and that now that I have the answers, I can make the best medical choices for me and my family.
Words by Anna De Souza.
Got a story tip or just want to get in touch? Email us at lifestyle.tips@verizonmedia.com

 Yahoo Lifestyle
Yahoo Lifestyle 

